What is Keratitis?
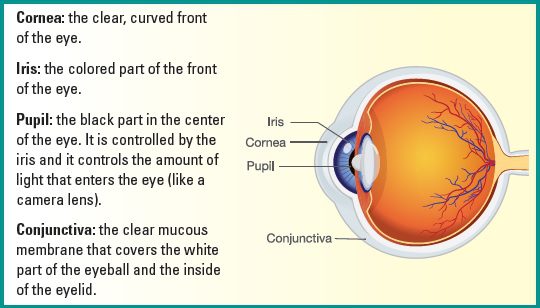
Keratitis (also known as “corneal ulcer”) is an inflammation of the cornea – the clear, dome shaped window located at the front of the eye that covers the iris and pupil. Keratitis resulting from infections (called infectious keratitis) can be caused by bacteria, viruses, fungi, and parasites. Keratitis can also occur a result of other insults to the cornea (called noninfectious keratitis) such as an injury, wearing your contact lenses too long, or very dry eye. Keratitis can become serious quickly – see your eye doctor right away to prevent vision loss.
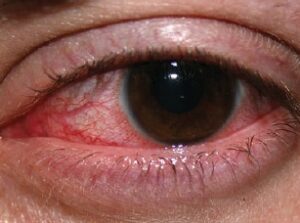
Conjunctivitis (also known as “pink eye”) is an inflammation of the the conjunctiva. This condition has similar symptoms and may be confused with keratitis. If you have keratitis symptoms as described on this page, see your eye doctor right away.
 Conjunctivitis (pink eye)
Conjunctivitis (pink eye)
What Causes Keratitis?
Keratitis can be infectious or non-infectious.
Infectious keratitis
Parasitic (Acanthamoeba) infection
Bacterial infections: Bacterial keratitis is common in people who wear contact lenses. Bacteria can grow on your contact lenses or contact lens case if you do not clean and store them properly. The bacteria can also come from contaminated eye drops or contact lens solution. It is more likely to occur if you wear extended-wear contact lenses (contact lenses that you sleep in).
Viral infections: Keratitis from a viral infection is usually due to the herpes simplex virus, the chicken pox virus, or the common cold. If you’re sick, be careful about touching your eyes and keeping your hands clean. If you have a cold sore (the herpes simplex virus), you can spread it by touching your sore and then your eye. The virus that causes cold sores may cause repeated keratitis infections. The repeated infections are triggered by stress, an impaired immune system, or exposure to sunlight.
Fungal infections: This type of keratitis infection is not common. It can be caused by scratching your eye with a branch or plant material. It can also be caused by the improper use of contact lenses or steroid eye drops.
Parasitic (Acanthamoeba) infection: Acanthamoeba are microscopic, single-celled organisms called amoeba. They are the most common amoebae found in fresh water and soil. The two biggest risk factors to get an Acanthamoeba infection are poor contact lens hygiene and exposure to water (like swimming pools and hot tubs) while wearing contact lenses.
Non-infectious keratitis
 Non-infectious keratitis
Non-infectious keratitis
Injury: Scratches, scrapes and cuts to your cornea can cause noninfectious keratitis. These injuries can happen from a variety of sources, such as fingernail scratches, paper cuts, makeup brushes, tree branches, contact lenses, and chemical burns. The injury may also let in bacterial or fungus to cause an infectious keratitis.
Eyelid disorders that prevent proper eyelid function: If the eyelid does not close properly, the cornea can dry out, and keratitis can develop.
Dry eye syndrome: The eyes are not able to leave a protective layer of tears (called the tear film) that washes, soothes and protects the eye every time you blink. The eye then becomes dry and irritated which can lead to keratitis.
Exposure to intense ultraviolet (UV) light (photokeratitis): Photokeratitis is caused by damage to the cornea by UV light. It can be caused by the reflection of UV light from the sun from sand, water, ice and snow; looking directly at a solar eclipse without eye protection, tanning beds, and/or welding.
What are the Symptoms of Keratitis?
The first sign and symptoms of keratitis is usually eye pain, redness, and blurred vision. Your eye may burn or feel irritated, or it may feel like you have something in it. Signs and symptoms of keratitis include:
- Eye pain
- Eye redness
- Excess tears or other discharge from your eye
- Difficulty opening your eyelid because of pain or irritation
- Blurred vision
- Decreased vision
- Sensitivity to light (also called photophobia)
- A feeling that something is in your eye
Keratitis can cause permanent vision loss, so see your eye doctor right away if you have any of these symptoms.
What Increases the Risk for Keratitis?
You may be at increased risk for keratitis if you:
• Wear contact lenses: Wearing contact lenses (especially sleeping in the lenses) increases your risk of both infectious and noninfectious keratitis.
The risk increases from:
-
- Wearing them longer than recommended
- Improper disinfection
- Wearing contact lenses while exposed to water (like swimming pools or hot tubs)
- Have reduced immunity: If your immune system has been weakened by disease or medications, you are at a higher risk of developing keratitis.
- Use steroid eye drops: Use of steroid eye drops to treat an eye disorder can increase your risk of developing infectious keratitis or worsen existing keratitis.
- Have an eye injury: If one of your corneas has been damaged from an injury, you may be more vulnerable to developing keratitis.
- Have or have had cold sores, chicken pox, or shingles
- Have dry eye
- Have an eyelid disorder that prevents proper functioning of the eyelid
- Not wearing proper eye protection (such as sunglasses, welding mask, etc.) to avoid exposure to UV light
If you wear contact lenses: Safe handling, storage and cleaning of your contact lenses are key steps to reduce your risk of keratitis. It is important to learn how to take care of your contact lenses. For more information, visit: https://www.preventblindness.org/wearing-contact-lenses.
How is Keratitis Diagnosed?
If you notice any of the signs or symptoms of keratitis, make an appointment to see your eye doctor right away. If you wear contact lenses, do not wear them until you find out what is wrong. Bring your contact lenses and contact lens case with you to the eye exam. Delays in diagnosis and treatment of keratitis can lead to serious complications, including blindness.
At your eye exam, the eye doctor will perform the following tests:
- History: The eye doctor will take a medical history, identify any illness, and ask you about your symptoms before examining your eye. • Visual acuity: This test will show how well you can see.
- Penlight exam: The eye doctor may examine your eye using a penlight, to check your pupil’s reaction, size, and other factors.
- Slit-lamp: The eye doctor uses a special microscope called a slit lamp. It shines a light into one eye at a time so the doctor can look closely at the outside and inside of the eye. Your eye doctor may apply a stain (fluorescein) to the surface of your eye, to light up any damage to your cornea.
- Laboratory analysis: The eye doctor may swab under your eyelid to get a sample of tears or some cells from your cornea for laboratory analysis. The doctor might also swab your contact lens case as a separate sample for analysis. This will help to determine the cause of keratitis and develop a treatment plan for your condition.
How to Treat Keratitis?
Noninfectious keratitis
A very mild case of noninfectious keratitis will usually heal on its own. For mild cases, your eye doctor may recommend that you use artificial tear drops. If your case is more severe and includes tearing and pain, you may need to use antibiotic eye drops to help with symptoms and prevent infection. For information on how to properly take eye drop medications, visit: https://www.preventblindness.org/taking-eye-drop-medications.
Infectious keratitis
Treatment of infectious keratitis varies, depending on the cause of the infection.
- Bacterial keratitis: Depending on the severity of your infection, antibiotic eye drops may be used for mild cases. In moderate to severe cases, you may also need to take oral antibiotics treat the infection.
- Fungal keratitis: You would need to take antifungal eye drops and oral medication.
- Viral keratitis: You may need artificial tear drops, antiviral eye drops and/or oral antiviral medications.
- Acanthamoeba keratitis: This keratitis may be difficult to treat. You may be prescribed antibiotic drops. If you have a severe case, a corneal transplant may be needed.
Your eye doctor may also prescribe steroid eye drops (never with fungal keratitis) after your infection has improved or is gone. These drops help to reduce swelling and help prevent scarring. You should only use steroid eye drops under close supervision by your eye doctor because steroid eye drops can sometimes make an infection worse.
Surgical Treatment
A corneal transplant replaces a damaged cornea with a healthy donor cornea. You may require a corneal transplant if you have the following:
- Keratitis that does not respond to medication
- Corneal scarring that greatly impairs your vision
What Causes Vision Loss from Keratitis?
Keratitis, if caught early, is usually easy to treat and clears up quickly. Corneal scarring is the most common complication of keratitis, which can lead to vision loss. If keratitis is not treated in a timely manner, the infection could go through the cornea and spread to other areas of the eye leading to possible blindness. It is important to see any eye doctor as soon as symptoms of keratitis are noticed.
How to Prevent Keratitis?
If you are sick, wash your hands often and try not to touch your eyes. Wear proper eye protection if you are looking at intense UV light. And if you wear contact lenses, handle and care for them correctly:
- Follow your eye doctor’s recommendations for taking care of your contact lenses
- Wash your hands and make sure they are completely dry before touching your contact lenses or your eyes
- Always use fresh solution to clean and store your contact lenses
- Keep the area where you store and keep your contact lenses and contact lens case clean and germ free
- Never store contact lenses in tap water
- Do not sleep in contact lenses when you are supposed to take them out every night
- Do not swim or shower in your contact lenses
- Replace your contact lenses and contact lens storage case as recommended
Resources for Eye Care
Prevent Blindness has a list of financial assistance resources for those in need of support in meeting their eye health needs and medications. Visit: www.preventblindness.org/visioncare-financial-assistance-information.

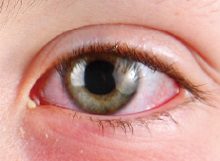 Conjunctivitis (pink eye)
Conjunctivitis (pink eye)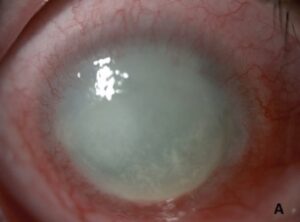
 Non-infectious keratitis
Non-infectious keratitis